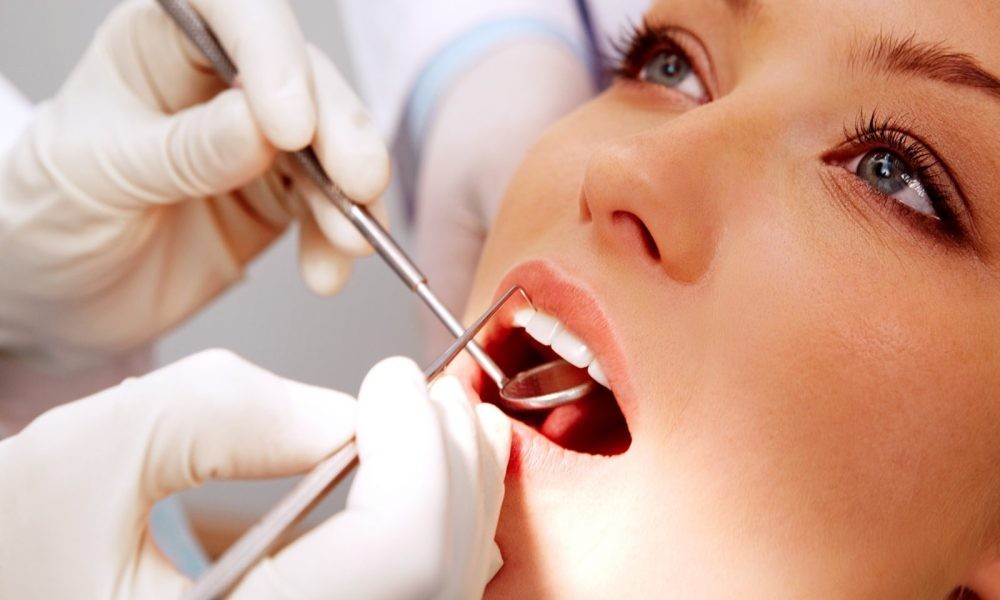
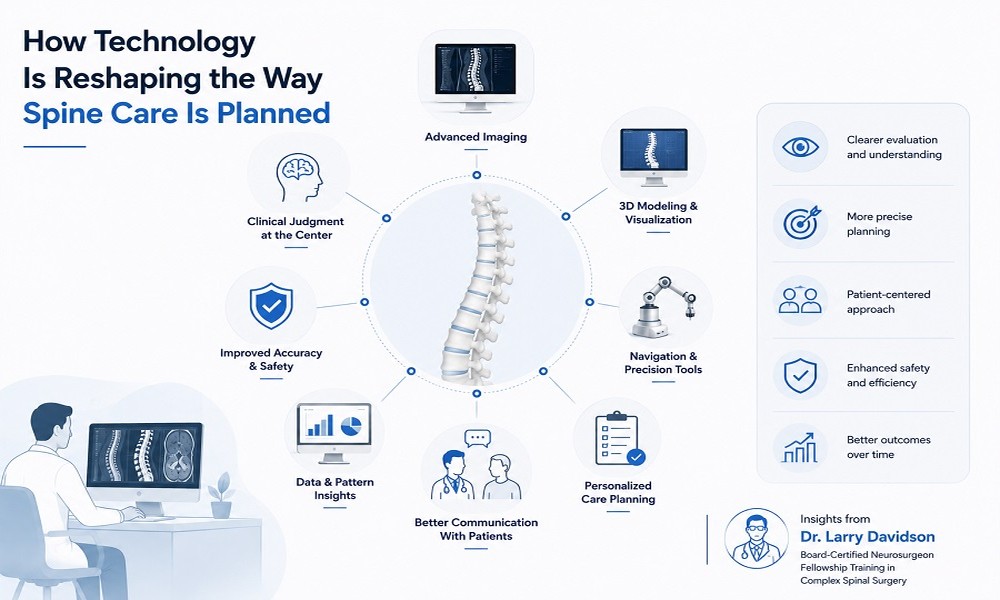
Exploring the Oral-Facial Wellness Relationship
Many view a bright smile as a simple cosmetic feature. In reality, the condition of teeth and gums is deeply linked to one’s overall physical state.
The mouth serves as a primary gateway to the body. Its status directly influences systemic wellbeing and facial aesthetics.
Maintaining optimal dental care is a cornerstone of preventative medicine. It affects numerous bodily systems, extending far beyond the jaw.
Contemporary science has transformed our understanding. We now know that issues within the mouth can signal or even fuel significant complications elsewhere.
This establishes pathways where bacteria and inflammation impact heart function, metabolism, respiration, and cognitive performance.
Therefore, dental professionals increasingly adopt a holistic perspective. They consider the wider implications of routine care.
Regular check-ups are thus crucial health screenings. They can uncover early indicators of broader systemic diseases.
This article will examine the evidence linking daily hygiene practices to outcomes like heart disease. It sets the rationale for a detailed exploration.
Key Takeaways
- The mouth acts as a critical gateway, influencing overall bodily systems and facial appearance.
- Optimal dental care is a fundamental component of preventative healthcare, not merely a cosmetic concern.
- Modern research reveals oral conditions can signal or contribute to serious systemic health complications.
- Bacteria and inflammation from the mouth can affect cardiovascular, metabolic, respiratory, and cognitive function.
- Dental professionals now view care through a holistic lens, considering whole-body implications.
- Routine dental appointments act as essential health screenings that can detect early disease warnings.
- Evidence demonstrates clear links between oral hygiene and conditions like heart disease and pregnancy issues.
Oral Health and Facial Wellness Connection: An Overview
A landmark report from two decades ago fundamentally reshaped how professionals perceive dental care. It moved the focus from isolated teeth towards a more integrated view of bodily function.
Defining the Connection
This integrated view considers all anatomical components. It includes gums, bones, ligaments, muscles, glands, and nerves.
These structures work together to enable essential human functions. They allow people to speak, smile, taste, and chew food effectively.
Perhaps most importantly, they are the foundation for conveying emotions through facial expressions. This function is central to communication and psychological wellbeing.
Key Research Insights
The pivotal 2000 Surgeon General’s report, Oral Health in America, catalysed this shift in understanding. It framed dental status as a critical component of overall physical state, not a separate concern.
The report established that the mouth’s condition serves a dual role. It acts as both an indicator of systemic health and a potential contributor to broader disease processes.
Subsequent research has documented the physiological mechanisms behind this link. Inflammation and bacteria in the mouth can create pathways affecting other bodily systems.
This evidence underscores why dental status is now viewed through a holistic lens. Managing oral conditions is recognised as a key part of maintaining general wellbeing.
The Mouth-Body Relationship: Systemic Implications
Within the complex ecosystem of the mouth lies a direct communication channel to the body’s vital system. This mouth-body connection reveals the mouth as an integrated part of the whole organism. It is not an isolated anatomical region.
This mouth-body connection operates as a two-way street. Conditions in the mouth can signal issues elsewhere. Systemic problems often manifest orally. Good oral health is thus a cornerstone of general wellbeing.
How Bacteria Influence Overall Health
The human mouth harbours over 700 species of bacteria. These bacteria form a sophisticated ecosystem. A delicate balance exists between beneficial and harmful bacteria.
Poor hygiene disrupts this equilibrium. Harmful bacteria then multiply, creating conditions for disease. Inflamed gum tissue provides a gateway for these microbes.
Through this gateway, bacteria can enter the bloodstream. Once in the bloodstream, they travel to distant organs. This migration triggers inflammatory responses throughout the body.
Chronic exposure to oral bacteria sustains systemic inflammation. The body’s immune system responds to this invasion. Managing the microbial balance in the mouth is fundamental for protecting overall health.
Gum Disease, Inflammation and Facial Aesthetics
Periodontal conditions represent more than just a dental issue; they are a source of chronic inflammation with far-reaching consequences. This process directly undermines both systemic wellbeing and the structural support for one’s smile.
The visible signs, such as receding gums or loosening teeth, often point to deeper health concerns.
Understanding the Impact of Inflammation
Gum disease begins when poor oral hygiene allows plaque bacteria to thrive. The body’s immune system attacks this buildup, causing inflammation in the gum tissues.
This initial stage, called gingivitis, makes gums red, swollen, and prone to bleeding. If untreated, the inflammation spreads deeper.
It destroys the fibres and bone anchoring teeth, advancing to periodontitis. This disease creates pockets where bacteria accumulate further.
Crucially, the inflammation is not contained. Inflammatory mediators from the infected gum tissues enter the bloodstream.
They circulate, contributing to inflammatory conditions elsewhere in the body. Chronic gum disease thus fuels a state of systemic inflammation.
Locally, persistent infection erodes the jawbone. This bone resorption can alter facial contours, leading to a sunken appearance over time.
| Stage | Primary Focus | Tissue Impact | Systemic Link |
|---|---|---|---|
| Gingivitis | Bacterial plaque on gum line | Inflamed, bleeding gums; reversible damage | Localised inflammation; minimal systemic spread |
| Periodontitis | Deepening infection and pocket formation | Bone loss, gum recession, tooth mobility | High levels of inflammatory markers enter circulation |
| Advanced Disease | Significant structural destruction | Tooth loss, major bone resorption, facial change | Strong contributor to chronic systemic conditions |
Controlling this inflammatory cascade is therefore vital. Effective management protects both facial structure and overall health.
Comprehensive Dental Care and Systemic Wellbeing
A modern dental appointment is far more than a simple check-up for cavities. It represents a proactive strategy for safeguarding one’s overall physical state. This approach, known as comprehensive dental care, views the mouth as a window to the body’s systemic condition.
Thorough examinations form its foundation. Using digital radiography and full-mouth assessments, clinicians can detect subtle early signs. These signs may point to issues extending beyond the gums and teeth.
Preventative Strategies in Dental Practice
Periodontal therapy exemplifies this dual-purpose philosophy. It addresses local disease while actively reducing the body’s inflammatory burden. This directly supports systemic wellbeing.
Key clinical interventions include:
- Professional cleaning (scale and polish) to disrupt harmful bacterial biofilms.
- Fluoride applications that strengthen enamel and prevent decay.
- Antimicrobial treatment to control specific pathogenic populations.
Empowering individuals through education is another critical component. It helps people understand the tangible links between their daily hygiene and broader oral health outcomes.
Consequently, regular visits function as essential preventative screenings. Trained professionals can identify warning signs for patients, potentially flagging systemic concerns like diabetes during routine care. This positions dentistry as a vital partner in maintaining long-term health.
Integrating Skincare into Oral Health Management
A truly holistic view of facial aesthetics requires attention to both dermatological and dental factors simultaneously. Progressive practitioners recognise that optimal appearance and wellbeing are achieved through coordinated strategies.
Skin condition and the state of one’s mouth share common influencing factors. These include inflammation levels, bacterial balance, nutritional status, and lifestyle behaviours.
Innovative Approaches by “Banning Skin Ltd”
Forward-thinking clinics exemplify this integration. Programmes by Banning Skin Ltd, for instance, combine dermatological assessments with dental considerations.
This approach ensures treatments address the face as a unified system. It moves beyond isolated concerns.
Benefits of Combining Skincare and Dental Care
This synergy offers clear advantages for patients. Key benefits include:
- Improved treatment outcomes: Managing oral inflammation can enhance facial skin appearance.
- Enhanced aesthetic results: A healthy gum line and strong teeth are foundational for a confident smile, which complements clear skin.
- More comprehensive understanding: A coordinated care team can identify issues one discipline might miss.
Ultimately, integrating these fields supports overall wellness. It positions daily dental care and skincare as complementary pillars of a unified health strategy.
Advanced Dental Techniques for Holistic Health
Contemporary dentistry has evolved beyond fillings and extractions to embrace a whole-body philosophy. This approach uses sophisticated tools to assess the mouth as a mirror of general wellbeing.
Advanced techniques now reflect integrated health principles. They treat individuals as complete systems rather than focusing on isolated symptoms.
Modern Treatment Modalities
Cutting-edge technologies enable more precise diagnostics and effective interventions. These include advanced imaging systems and laser therapies.
Minimally invasive procedures and biological treatments improve outcomes. They also reduce patient discomfort and recovery time.
Such modalities allow earlier detection of both local disease and systemic conditions. Timely intervention prevents progression to serious complications.
Preventive Check-Ups
Thorough examinations are vital for proactive care. Clinics like Banning Dental exemplify comprehensive protocols.
These check-ups screen for oral conditions while identifying indicators of broader issues. Patients can expect oral cancer screenings and periodontal assessments.
Bite evaluations and medical history discussions reveal crucial links. Personalised treatment plans are then developed by an experienced team.
This addresses individual risk factors rather than applying a one-size-fits-all approach.
| Technique | Primary Application | Benefit for Holistic Health |
|---|---|---|
| Digital Imaging (CBCT) | 3D visualisation of bone and teeth | Detects hidden infections impacting systemic health |
| Laser Therapy | Precise soft tissue treatment | Reduces inflammation with minimal trauma |
| Minimally Invasive Surgery | Tooth preservation procedures | Promotes faster healing and overall wellbeing |
| Biological Treatments (e.g., PRF) | Enhancing tissue regeneration | Supports the body’s natural healing processes |
Coordinated plans integrate multiple treatments and preventive strategies. This supports holistic health objectives effectively.
Oral Infections and Their Wider Health Risks
A severe tooth infection can quickly escalate from a localised problem to a threat against the entire body. Dental abscesses and other oral infections create reservoirs of harmful bacteria.
If these pathogens enter the bloodstream, they can cause sepsis. This life-threatening condition overwhelms the immune system.
Chronic infections also fuel systemic inflammation. This process contributes to cardiovascular disease and respiratory complications.
People with diabetes face particular risks. Poorly controlled oral infections can disrupt blood sugar management.
The mouth can serve as an early warning system. Lesions may indicate underlying systemic conditions like HIV.
Prompt treatment is therefore crucial. Delays allow bacterial proliferation and increase the risk of dissemination.
| Type of Oral Infection | Primary Systemic Risk | Mechanism of Spread |
|---|---|---|
| Dental Abscess | Sepsis, Endocarditis | Direct invasion into bloodstream |
| Advanced Periodontitis | Cardiovascular disease, Pneumonia | Chronic inflammation, aspiration of bacteria |
| Oral Candidiasis | Systemic fungal infection | Indicates compromised immunity |
| Pericoronitis | Ludwig’s Angina, Airway obstruction | Local spread to deep neck spaces |
This table illustrates how local infections link to major health issues. Managing dental problems protects overall health.
Preventing these conditions is a key part of holistic care. Regular dental check-ups are essential for early detection.
The Impact of Diet and Lifestyle on Oral and Facial Health
Lifestyle habits extend their influence far beyond weight management. They directly shape the condition of teeth and facial tissues. What people consume and their daily routines are powerful determinants of oral health overall.
Diets high in refined sugars and acids create an ideal environment for decay. When combined with poor oral hygiene, this accelerates gum disease and causes bad breath.
Nutritional Strategies for Optimal Wellness
Specific nutrient shortages manifest clearly in the mouth. A lack of vitamin C can lead to bleeding gums. Deficiencies in vitamin D or calcium weaken teeth and slow healing.
Other lifestyle factors also play a major role. Smoking, excessive alcohol, chronic stress, and poor sleep quality all compromise health overall. They increase systemic inflammation and infection risk.
Implementing positive nutritional strategies supports a resilient smile. Key dietary approaches include:
- Consuming calcium-rich foods like dairy or leafy greens to strengthen enamel.
- Eating crunchy vegetables (e.g., carrots, celery) that help clean surfaces naturally.
- Drinking adequate water to maintain saliva flow, which neutralises acids and washes away food particles.
This evidence shows that protecting oral health requires a comprehensive lifestyle approach. It integrates smart nutrition, consistent hygiene, and stress management for lasting health benefits.
Research and Emerging Trends in Oral-Facial Wellness
Recent findings from major health institutions have solidified the link between periodontal disease and serious systemic complications. This research transforms our understanding of preventative care.
Recent Findings from Institutional Studies
Studies show people with gum disease face a 20-50% higher risk for heart disease. Harmful oral bacteria can attach to arterial plaques, contributing to blockages.
A powerful bidirectional relationship exists with diabetes. Diabetics have three times the risk of severe gum disease. Conversely, this inflammation makes blood sugar control very difficult.
Maternal health is critically affected. Pregnant women with untreated gum issues face seven times the risk of premature delivery. This highlights the vital need for dental care during pregnancy.
Over 35,000 cases of oral and pharyngeal cancers are diagnosed annually. This results in roughly 8,000 deaths each year. Regular screenings are essential.
Emerging research explores connections to cognitive decline. Specific oral bacteria have been found in the brain tissue of Alzheimer’s patients. This opens new avenues for understanding neurodegenerative conditions.
These discoveries, built over many years, underscore the mouth’s role as a window to the whole system. They guide more integrated approaches to managing these conditions.
Conclusion
The evidence is clear: caring for one’s mouth is a direct investment in the entire body’s resilience. Decades of rigorous science confirm this link is measurable, not theoretical.
Maintaining optimal dental status safeguards against serious conditions affecting the heart, brain, and metabolism. It makes routine care a fundamental preventative strategy.
People have substantial control over outcomes through daily hygiene and smart lifestyle choices. Regular check-ups with a professional team act as essential health screenings.
These appointments can identify early warnings for systemic issues. An integrated approach, where dental and medical practitioners collaborate, offers the best protection.
Prioritising consistent oral hygiene and scheduling preventive examinations are crucial steps. This investment enhances quality of life and prevents complications.